Trauma Release Through Reflex Integration: Rebuilding the Nervous System from the Inside Out
When Stress Becomes Stuck in the Nervous System
Trauma is not simply an emotional experience—it is a neurologic and biochemical event that lives in the body. When the nervous system experiences overwhelming stress, it does not always resolve cleanly. Instead, the body can remain in a prolonged state of protection, even when the danger has passed.
For both children and adults, this shows up in ways that are often misunderstood. These are not simply behavioral issues. They are signs of a nervous system that has not completed its stress response cycle.
Trauma release is often associated with major, visible events. But for many children, stress begins much earlier and in much quieter ways—through medical experiences, sensory overwhelm, or a nervous system that is constantly working harder to interpret the world.
Children who are born prematurely, who have complex medical needs, or who are on the autism spectrum often experience stress not as a single event, but as an ongoing state within the nervous system.
For these children, early life may include:
Extended NICU stays with repeated medical procedures
Separation from caregivers during critical bonding periods
High levels of sensory input (lights, sounds, touch) before the nervous system is ready
Frequent transitions, therapies, or unpredictable routines
A nervous system that processes sensory information differently, leading to overload
Even when these experiences are necessary or life-saving, the nervous system still registers them as stress. The body does not interpret intention—it interprets input.
This creates a pattern where the stress response system is activated repeatedly, often before the nervous system has developed the capacity to regulate and recover.
Over time, this may look like:
Persistent startle or sensitivity to sound and touch
Difficulty settling, sleeping, or calming
Strong emotional reactions or withdrawal
Challenges with attention, coordination, and body awareness
A baseline state of hypervigilance or shutdown
At the same time, there is another layer of stress that is often overlooked—the stress carried by caregivers.
Parents of children with high needs are navigating:
Constant vigilance and decision-making
Emotional strain of medical or developmental uncertainty
Sleep disruption and physical exhaustion
Advocacy within medical and educational systems
The weight of wanting to help, without always having clear answers
Research suggests that approximately 1 in 5 parents of children with autism have symptoms consistent with PTSD. This is not a reflection of weakness—it is a reflection of prolonged, unrelenting stress without adequate resolution.
When both the child and caregiver are living in states of chronic activation, the nervous system becomes organized around survival rather than connection, growth, and regulation.
This is where understanding trauma release becomes essential.
Because trauma is not just what happened—it is what the nervous system is still holding.
Understanding trauma release requires us to move beyond behavior and into the biology of the nervous system—specifically how stress, reflexes, and regulation are deeply interconnected.
The Nervous System Mechanism: Stress as a Neurologic and Biochemical Response
Stress begins as a survival response. When the brain perceives a threat—whether physical or emotional—it activates a cascade of neurologic and biochemical reactions designed to protect the body.
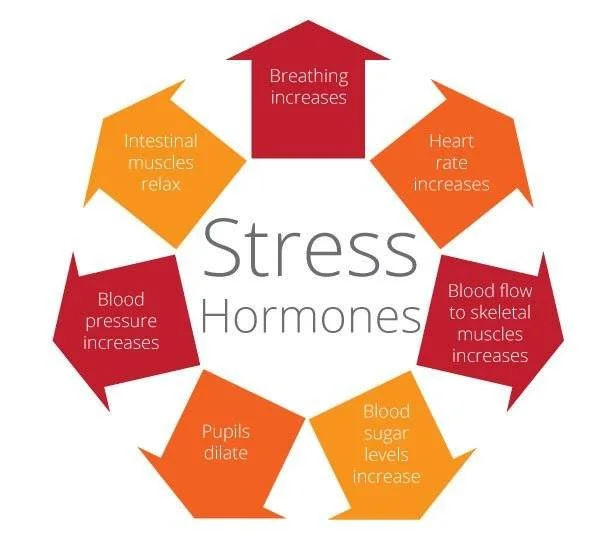
This response is primarily driven by the release of stress hormones, including:
Cortisol – mobilizes energy and increases alertness
Adrenaline (epinephrine) – prepares the body for immediate action (fight or flight)
Norepinephrine – sharpens focus and vigilance
These hormones are essential for survival. They increase heart rate, sharpen attention, and prepare muscles for action. However, they are designed to be temporary.
To return to a regulated state, the body relies on inhibitory and balancing neurochemicals:
GABA (gamma-aminobutyric acid) – calms neural activity and reduces excitability
Serotonin – supports mood stability and a sense of safety
Dopamine – supports motivation, reward, and adaptive movement
When the nervous system is functioning well, there is a balance between activation (stress hormones) and inhibition (regulating neurotransmitters).
Trauma disrupts this balance.
Instead of cycling through activation and returning to calm, the nervous system becomes “stuck” in a protective state. Stress hormones remain elevated, while calming neurotransmitters are underutilized or dysregulated.
This is where trauma becomes embodied.
The Role of the HPA Axis: Detecting Threat and Safety
At the core of the stress response is the HPA axis (Hypothalamic-Pituitary-Adrenal axis).
This system acts as the body’s central command for stress regulation:
The hypothalamus detects a threat
The pituitary gland signals the body to respond
The adrenal glands release cortisol and adrenaline
The HPA axis is constantly scanning for safety or danger. It does not differentiate well between physical threat and perceived emotional threat.
For a child, this means:
A loud noise
A sudden transition
A social demand
A feeling of uncertainty
can all activate the same stress response as a true physical danger.
When the HPA axis is overactive, the body begins to interpret neutral or mildly challenging situations as threats. This leads to chronic activation and difficulty returning to a baseline state.
The Role of the RAS: Filtering the World Through Threat
Another key system involved in trauma is the Reticular Activating System (RAS).
The RAS is responsible for filtering sensory information and determining what the brain pays attention to. It acts as a gatekeeper between the external world and internal awareness.
When the nervous system is regulated, the RAS filters appropriately:
It prioritizes relevant information
It ignores unnecessary stimuli
It allows for focused attention
However, under chronic stress, the RAS becomes biased toward threat detection.
This results in:
Heightened sensitivity to sound, touch, or movement
Difficulty focusing due to constant scanning
Overreaction to minor stimuli
A persistent sense of “something is wrong”
The RAS, like the HPA axis, begins to reinforce a narrative of danger.
This creates a feedback loop:
The body feels unsafe → the brain looks for threat → the body becomes more activated.
What Infant Reflexes Are—and Why They Matter
To understand trauma release through reflex integration, we must understand the role of infant reflexes.
Infant reflexes are automatic, involuntary movement patterns present at birth. They are the nervous system’s earliest tools for survival and development.
Examples include:
Moro reflex (triggering a fight or flight response)
Tonic Labyrinthine Reflex (TLR – preparing body’s posture for movement)
Asymmetrical Tonic Neck Reflex (ATNR- alerting to auditory and visual information)
Tendon Guard reflex (alerting the muscles and tendon’s to get ready for engagement)
These reflexes are not meant to stay active indefinitely. They are designed to:
Build neural pathways
Support sensory-motor development
Lay the foundation for posture, coordination, and regulation
As the brain matures, these reflexes become integrated into more complex, voluntary movement patterns.
How Reflex Circuits Shape Emotional and Physiological Regulation
Reflexes do more than create movement—they create feedback loops within the nervous system.
Each reflex circuit sends information between:
Sensory receptors
The spinal cord
The brain
This feedback builds the foundation for:
Body awareness
Emotional regulation
Motor control
Cognitive development
When reflexes are well integrated, the nervous system develops a stable foundation. The body can interpret sensory input accurately and respond appropriately. When reflexes remain unintegrated or dysregulated, the feedback loop becomes inconsistent or protective.
This is where trauma and reflex patterns intersect.
Reflexes as a Tool for Stress Response
Reflexes are not the problem. They are the body’s solution to stress.
Reflexes Engage to Protect in Times of Danger
When a threat is perceived, reflexes activate automatically:
The Moro reflex triggers a startle and breath intake
The Tendon Guard reflex creates tension and withdrawal
The Fear Paralysis reflex can lead to freezing
These responses are immediate and necessary. They protect the body without requiring conscious thought.
When Protection Becomes “Negative Protection”
The problem arises when these reflexes do not resolve. Instead of activating and then integrating, they remain in a chronic state of readiness. This is referred to as negative protection.
Negative protection means:
The body continues to respond as if danger is present
Reflexes are easily triggered by minor stimuli
The nervous system cannot move into higher-level regulation
Observable behaviors include:
Startle responses to small noises
Difficulty relaxing muscles
Emotional overreactions
Avoidance or shutdown
Persistent anxiety
The nervous system becomes organized around protection instead of growth.
Why This Happens: The Nervous System Cannot Differentiate Past from Present
Trauma is not stored as a clear narrative. It is stored as sensory and motor patterns.
The body remembers:
The tension
The movement pattern
The chemical state
Without intervention, the nervous system cannot easily differentiate between past and present experiences. Which leads to:
Reactivity to non-threatening situations
Repetition of protective patterns
Difficulty accessing calm, flexible responses
The system is not choosing this. It is operating based on the pathways that were built during stress.
Using Reflex Integration for Trauma Release
Trauma release is not achieved through cognition alone. It requires accessing the body’s original language—movement and sensation.
Reflex integration uses targeted movement and tactile input to reorganize the nervous system.
How This Works Neurologically
Reflex-based interventions:
Activate sensory receptors in muscles and joints
Stimulate neural pathways between the body and brain
Support the function of interneurons
Interneurons are critical because they regulate communication between neurons. They play a key role in balancing excitation and inhibition.
Through this process, reflex integration helps restore:
GABA activity – calming excessive neural firing
Dopamine pathways – supporting motivation and adaptive response
Serotonin levels – increasing a sense of safety
This is not simply movement. It is targeted neurologic input designed to rebuild communication within the nervous system.
Building Stronger Neural Pathways
One of the primary goals of reflex integration is to support the maturation of the nerve net system.
This includes strengthening neural connections by supporting myelination (insulation of nerve pathways) to improving speed and efficiency of communication.
When pathways are weak or disrupted due to stress, the nervous system defaults to survival-based responses.
Reflex work helps rebuild:
Stable postural control
Coordinated movement patterns
Efficient sensory processing
Over time, this creates a foundation where regulation becomes more accessible.
Regulating the Tendon Guard System
The Tendon Guard reflex is particularly relevant in trauma.
This reflex is responsible for:
Protecting the body from perceived danger
Creating muscular tension
Preparing for withdrawal or defense
In chronic stress, this system becomes overactive.
Reflex integration uses:
Tactile input (specific touch patterns)
Neurostructural techniques
Guided movement patterns
to help the body experience safety within movement.
This allows the nervous system to reduce chronic tension by expanding movement options to shift from protection to adaptability.
Goals of the Masgutova Method in Trauma Release
The Masgutova Method provides structured protocols designed to support trauma recovery through reflex integration: Stress Hormone Release, PTSD protocol, Panic Attack Protocol and Basal Ganglia Regulation. While the protocols are all rooted in restoring balance to the nervous system through similar reflexes, the techniques differ to allow opening and growth in different brain systems.
Release Stored Stress Hormones
Through movement and tactile input, the body is given an opportunity to complete incomplete stress responses. This supports the release of Adrenaline and Cortisol allowing the system to move out of chronic activation.
Increase Sense of Safety Through Sensory Input
Touch and proprioceptive input are powerful regulators of the nervous system. These inputs help increase Serotonin (calm and safety) as well as Dopamine (engagement and motivation).
The body begins to experience safety not as a concept, but as a physical state.
Release Negative Protection
Negative protection keeps the nervous system locked in survival. Reflex integration helps decrease automatic protective responses; allow flexibility in movement and emotion; support progression into higher-level brain function.
Differentiate the “Here and Now” from the Past
As the nervous system reorganizes, it gains the ability to distinguish current sensory input from past stored patterns. This reduces reactivity and supports more appropriate responses to present situations.
Find Grounding and Stability
Through reflex work, the body develops: improved postural control, greater body awareness, increased ability to remain present
Grounding becomes a neurologic capacity, not just a strategy.
Activate the Brain’s Sense of Agency
One of the most important outcomes is the restoration of the belief:
“I can protect myself.”
This is not cognitive—it is embedded in movement and sensation.
When the body experiences successful, organized responses, the brain updates its internal model of safety.
Remind the Body It Can Stretch and Grow
Trauma creates contraction—physically and neurologically. Reflex integration introduces expansion, lengthening, controlled movement.
This reminds the nervous system that growth is possible beyond protection.
Observable Shifts as the Nervous System Reorganizes
As reflex-based trauma work supports the nervous system in moving out of protection and into regulation, changes begin to emerge across daily function. These shifts are not isolated skills—they reflect a deeper reorganization of the nervous system and its ability to process, respond, and recover.
In the area of regulation, individuals often demonstrate an increased ability to return to baseline after stress. Instead of remaining in prolonged states of activation or shutdown, the nervous system begins to cycle more efficiently. This may look like fewer and shorter emotional escalations, improved sleep patterns, and a greater capacity to tolerate transitions and unexpected changes.
In movement and posture, the body becomes less guarded. Chronic tension decreases, and movement patterns become more fluid and coordinated. You may observe improved balance, smoother motor planning, and a more stable postural foundation. These changes reflect improved communication between the brain and body, rather than simply increased strength or practice.
From an emotional standpoint, there is often a noticeable increase in flexibility. Individuals may still experience stress, but they are less overwhelmed by it. There is greater access to adaptive responses, increased resilience, and a reduced tendency toward extreme reactions such as fight, flight, or freeze.
In cognitive and functional performance, improved regulation creates the conditions for engagement. Attention becomes more consistent, problem-solving improves, and individuals are better able to participate in learning, social interaction, and daily routines. These are not just cognitive gains—they are the result of a nervous system that feels safe enough to engage.
Together, these changes reflect a foundational shift: the nervous system is no longer organized primarily around protection, but is beginning to support growth, connection, and purposeful action.
Where True Trauma Release Begins
If you are seeing signs of chronic stress, reactivity, or dysregulation—whether in a child or yourself—look deeper than behavior.
The nervous system may be asking for support at its most foundational level.
Reflex integration offers a pathway to:
Restore regulation
Rebuild resilience
Create lasting change
True trauma release is not about forcing calm—it is about building a nervous system that can access it.
And when the nervous system has that foundation, everything else—learning, connection, and daily life—becomes more possible.
Moving Forward: From Protection to Possibility
The nervous system is not broken—it is adaptive.
What we often see as dysfunction is actually a system that has learned to survive under stress.
The goal is not to remove these protective responses, but to help the nervous system expand beyond them.
This begins with:
Understanding the role of stress in the body
Recognizing the impact of reflex patterns
Providing targeted, neurologically informed intervention
When the foundation changes, everything built on top of it can change.
Read how one young individual was able to move into recovery after one session of the PTSD protocol.
Returning to the Whole System: Why Trauma and Stress Hormone Release Matters for Both Child and Caregiver
When we consider trauma and stress through a neurologic lens, it becomes clear that many children—and their caregivers—are not starting from a neutral baseline. Their nervous systems have been shaped by repeated activation, often without the opportunity for full resolution.
For children who were premature, medically complex, or navigating autism, the stress response system may have been activated early and often. Reflex patterns may have organized around protection. The HPA axis may remain on high alert. The RAS may continue to scan for threat in environments that are objectively safe.
This is not a failure of development. It is the nervous system doing exactly what it was designed to do—protect.
But over time, this protective organization can limit access to higher-level skills:
Regulation becomes effortful
Learning requires more energy
Social engagement feels overwhelming
The body remains in patterns of tension or withdrawal
At the same time, caregivers who have lived in prolonged states of stress may also carry:
Elevated cortisol and adrenaline patterns
Difficulty fully relaxing, even in safe moments
Heightened emotional reactivity or fatigue
A nervous system that is primed for vigilance
This matters, because regulation is not an individual process—it is relational. A child’s nervous system is constantly interacting with the caregiver’s nervous system.
When both systems are supported, the potential for change expands.
Trauma and stress hormone release through reflex integration offers a pathway to address this at the foundation.
For the child, it helps:
Release stored patterns of stress and protection
Reorganize reflex circuits that are driving reactivity
Build a more stable internal sense of safety
Create the neurologic conditions for growth and learning
For the caregiver, it offers:
A way to understand their own stress responses through a biologic lens
Tools that support co-regulation through touch, movement, and presence
Opportunities for their own nervous system to shift out of chronic activation
This is not about “fixing” either system. It is about reorganizing nervous system that were shaped by experience – and recognizing the capacity of both to reorganize and change.
When the nervous system is given the right input, it can begin to:
Differentiate past from present
Reduce the intensity of protective responses
Access regulation more consistently
Support connection, resilience, and daily function
Children who began life in stress—and parents who have carried that stress alongside them—deserve support that reaches beyond behavior and into the nervous system itself.
True trauma release is not about forcing calm—it is about building a nervous system that can access it.
Because when we address the foundation, we create the possibility for something different:
A shift from surviving…
to truly, sustainably thriving.